The goals of the community engagement component of the CHNA are to:
- Identify San Franciscan’s health priorities, especially those of
vulnerable populations
- Obtain data on populations and issues for which we have little
quantitative data
- Build relationships between the community and SFHIP
- Meet the regulatory requirements including the IRS rules for Charitable
501(c)(3) Charitable Hospitals, Public Health Accreditation Board
requirements for the San Francisco Health Department, and the San
Francisco’s Planning Code requirements for a Health Care Services
Master Plan
The 2019 CHNA includes 4 categories of focus groups: SFHIP key informant
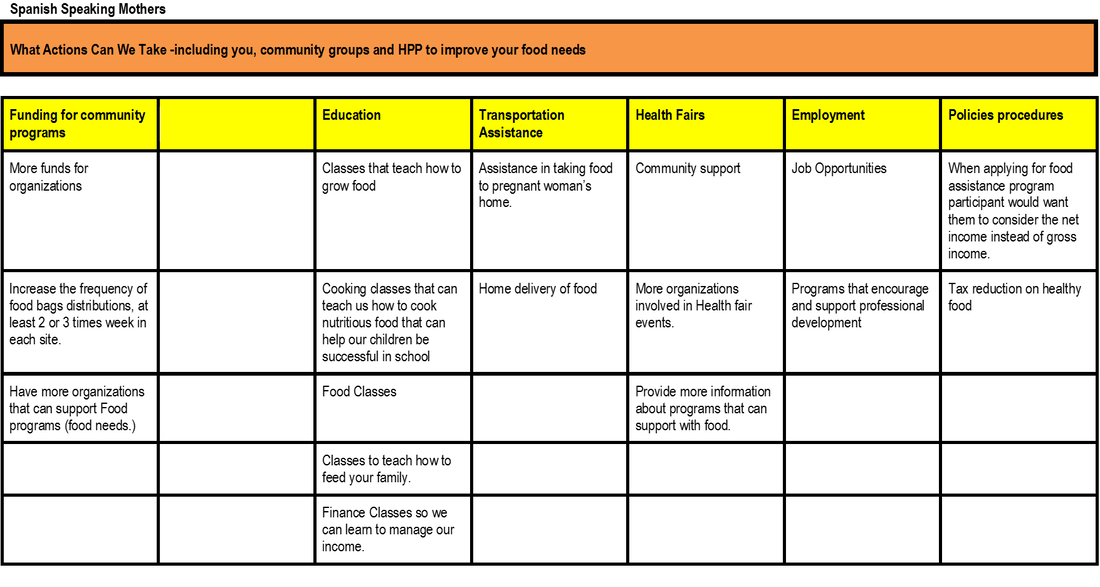
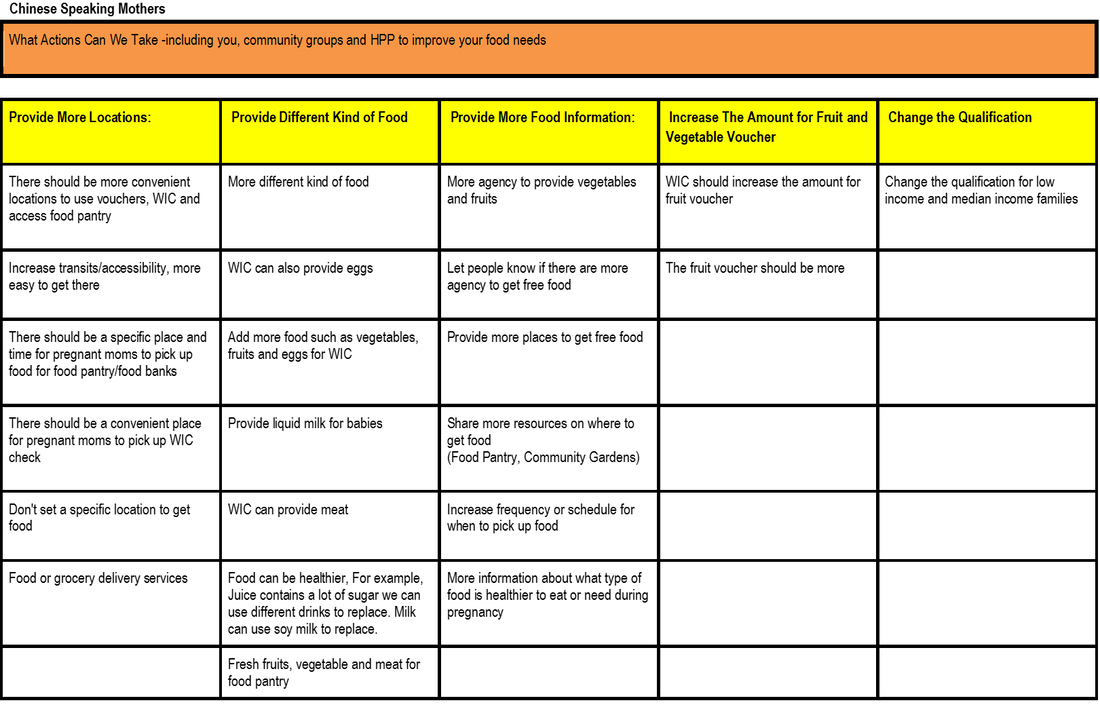
group interview, Equity Coalition focus groups, food insecure pregnant
women focus groups, and Kaiser focus groups.
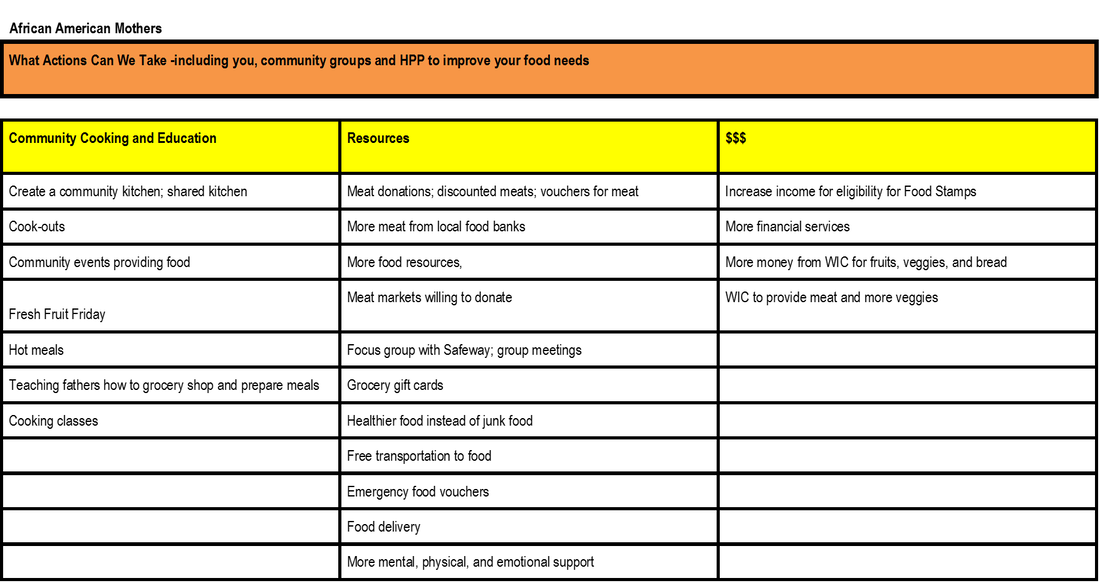
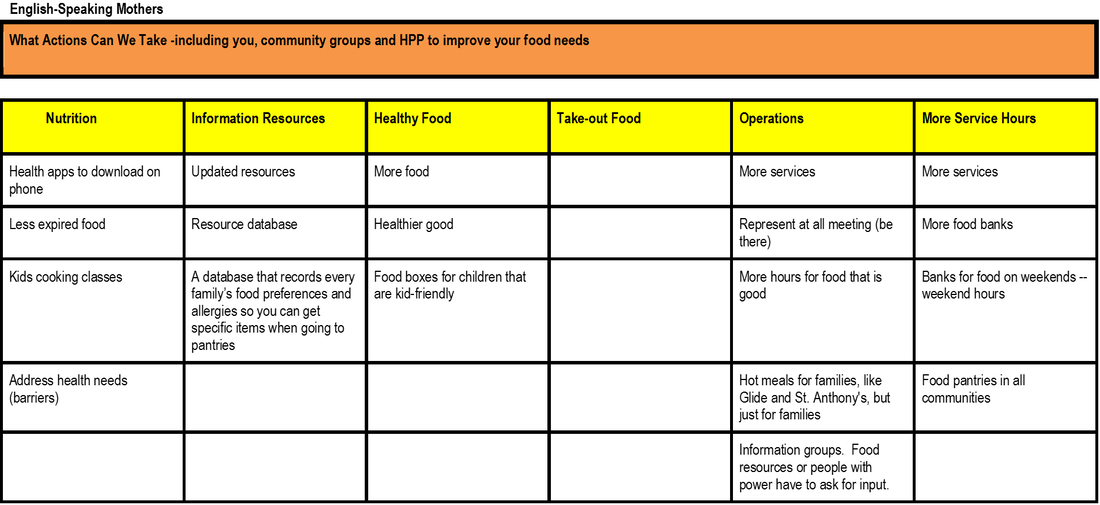
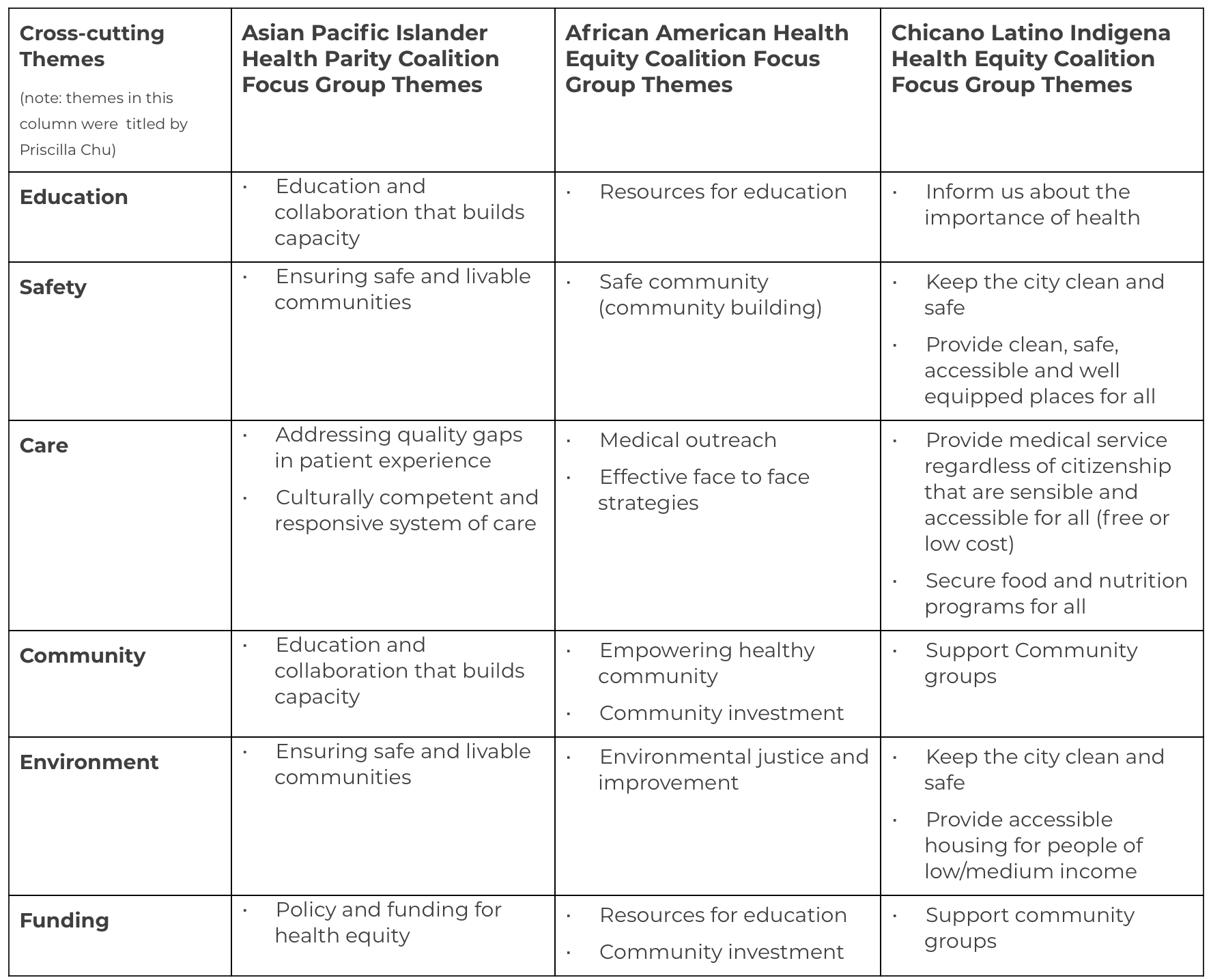
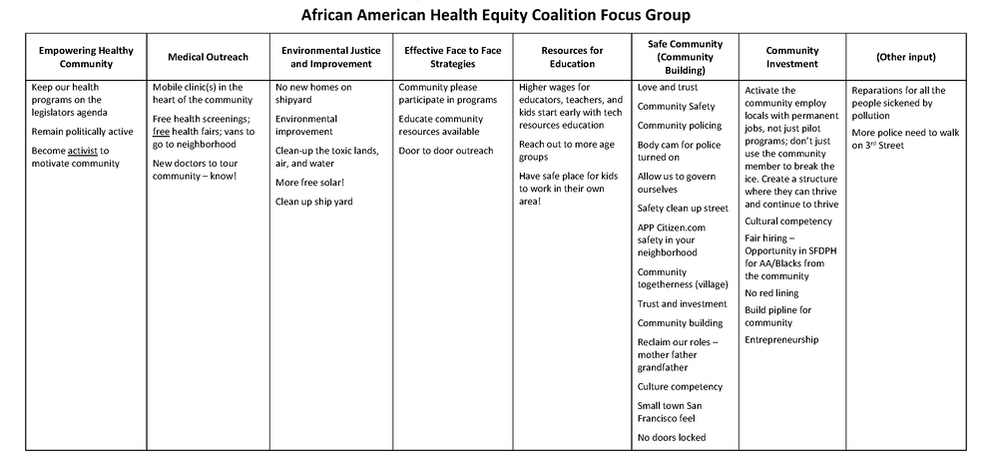
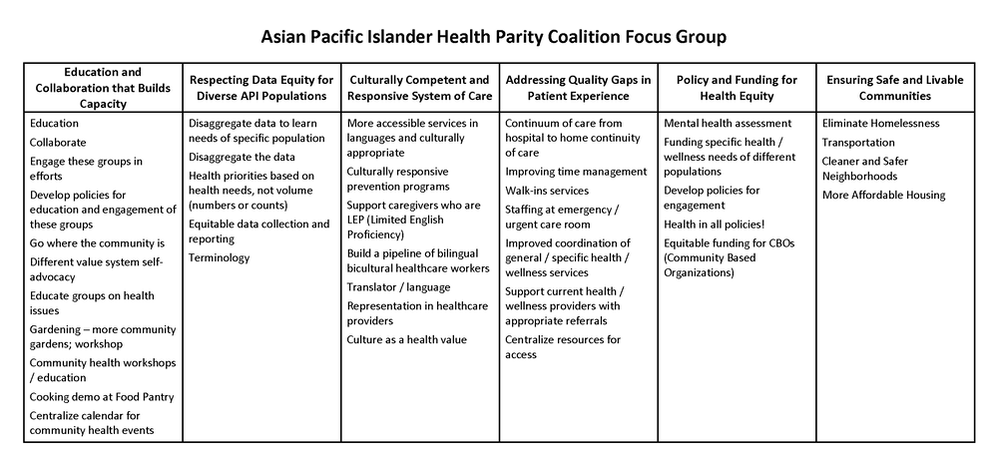
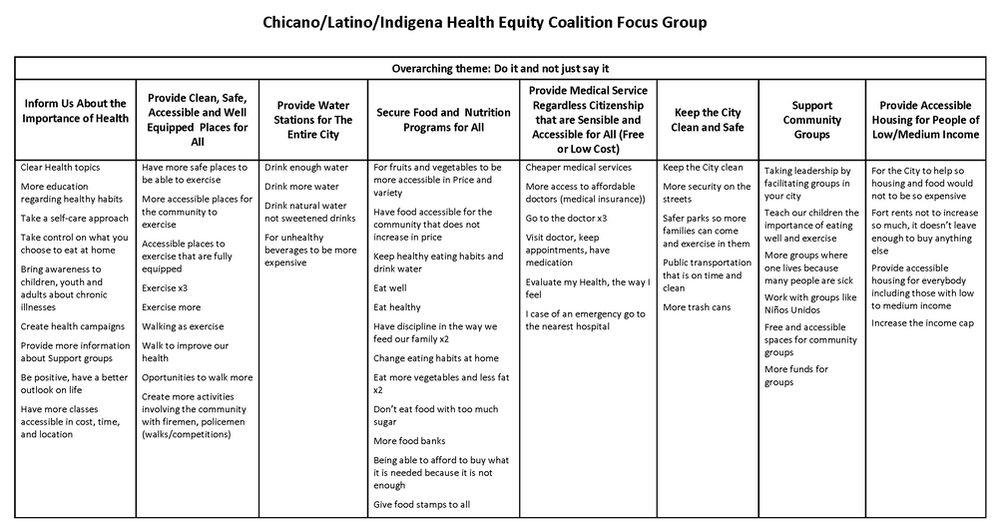
Equity Coalition focus groups. Focus groups were conducted with each of the three health equity coalitions in San Francisco: The Chicano / Latino / Indigena Health Equity Coalition, The Asian Pacific Islander Healthy Parity Coalition, and The African American Health Equity Coalition. The Asian Pacific Islander Healthy Parity Coalition focus group was comprised of care providers and executive directors of community based organizations that provided services to their community. The African American Health Equity Coalition hosted approximately 40 diverse and mostly Black / African American community members to attend their focus group. The Chicano / Latino / Indigena Health Equity Coalition invited Indigena promotoras, many of whom spoke Mayan as their first language, to participate in their focus group.
Using the Technology of Participation (ToP) Consensus Method, the question posed to each focus group was, “What actions can we take to improve health?”.While each focus group came up with their own particular themes, the broad cross-cutting themes from all three equity coalition focus groups covered education, safety, care, community, environment, and funding.